Stay updated with internal news from the university about our center's faculty, students, researchers, partners, and affiliates, highlighting their achievements and activities.
Center for Human Rights and Humanitarian Studies
Community Spotlight
Recent News
Eight scholars from Brown University looked back at the pandemic with an eye toward how its lessons can help the United States and other nations prepare for the next global health crisis.
Read Article
News from SPH
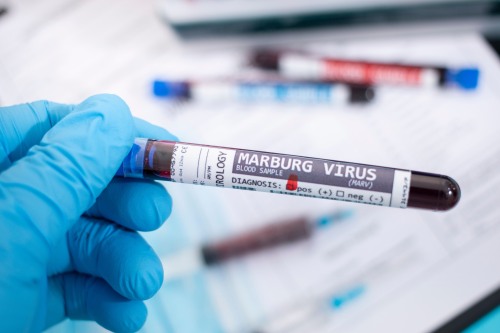
How Rwanda's health system stopped Marburg in its tracks
This fall there was a deadly disease outbreak in the east African country of Rwanda. But you may not have heard about it, and according to Professor Craig Spencer, that’s a good thing.
Read Article
“The Power of Faces,” an exhibition by two Rhode Island-based photographers on view through Dec. 20, displays portraits of people living in refugee camps across the world.
Read Article
In a major step toward expanded research and teaching, the new school will extend Brown’s commitment to advancing knowledge and preparing the next generation of global policymakers and leaders.
Read Article
The Center for Human Rights and Humanitarian Studies was named one of the partners to receive rapid research funding from the National Center for Disaster Medicine and Public Health in the event of a future disaster.
Read Article
The Center for Human Rights and Humanitarian Studies recently secured funding from the Pembroke Faculty Seed Grant for its research on "The Women, Peace and Security Agenda in the Middle East."
Read Article
Over winter break, ten Brown students learned the ins and outs of journalism focused on global issues and the nuances of international reporting in an evolving media landscape at the Center for Strategic and International Studies, a prestigious Washington, D.C. think tank. In one week, they learned more than they could have imagined.
Read Article
The Watson Institute awarded Birkelund funds to five faculty research projects during the 2023 - 2024 academic year. Projects ranged from studying civilian-military coordination during the pandemic to creating a study group between Brown students and faculty, and quilombola communities in Brazil.
Read Article
In a new paper, a team of researchers led by members of the Watson Institute's Center for Human Rights and Humanitarian Studies found that civil society organizations in the Global South played a critical role in response to the COVID-19 pandemic.
Read Article